Introduction
Bladder cancer is one of the most common cancers of the urinary system (1). Bladder urothelial cell carcinoma is a heterogeneous group of tumors with different malignant potentials (2, 3). Approximately 80% of bladder cancers are low-grade superficial tumors (4). Although superficial tumors are resected transurethrally, the recurrence rates of these tumors are high (60%-85%) (5). Fortunately, the five-year survival rate is high (80%-90%) (6), and that is why the biggest concern in patients with superficial bladder cancer is to reduce and procrastinate the recurrence and prevent the progression to invasive disease (7). Therefore, long-term follow-up is needed in these patients. Routinely, cystoscopy and cytology are used to diagnose and follow up superficial bladder tumors (8). Cystoscopy is the most efficient method available to detect primary or recurrent bladder cancer (9). Yet cystoscopy is an invasive procedure and causes some discomfort in patients, and it might be ineffective in diagnosing in situ or superficial tumors (9-11). Therefore, it is important to use urine cytology as a noninvasive complementary method (12, 13). Urine cytology is an important noninvasive diagnostic method for urinary tract cancers, especially carcinomas (13, 14). It has a 95% sensitivity and nearly 100% specificity in detecting high-grade urothelial malignancies (15). However, it is a low-sensitive method for detecting low-grade malignant urothelial tumors (the most common urothelial carcinoma) (16, 17). It is useful for follow-up in treated patients and to evaluate the residual of malignant bladder tumors after surgery (18). One of the recent methods is liquid-based cytology (LBC), which was used in cervical cytology for the first time (19). Urinary samples for LBC were centrifuged, and then the precipitates were transferred to a Cytolytic solution (Sina Dej Sahand Co, Tabriz, Iran). After the second round of centrifugation, two or three drops of precipitates were transferred to a preservative solution (Sina Dej Sahand Co, Tabriz, Iran). The vial and slide were placed in a ThinPrep processor (SHANDON, CYTOSPIN3, UK). Then, the preparation steps (i.e., dispersion, cell collection, cell transfer, and staining) were done.
Compared to direct smear cytology (DSC), LBC has lower background elements (such as cellular debris, inflammatory cells, and blood cells), provides better cell preservation, and has a higher satisfaction rate (20-22). In the LBC method, after adding the fixative solution, all extracted cells were maintained; therefore, there are more cells for cytological examination.
The purpose of this study was to evaluate urine cytology, detect bladder lesions with two different methods (i.e., direct smears and LBC), and determine the sensitivity and specificity of these methods.
Material and Methods
A total of 146 patients suspected of having bladder carcinoma were selected from Armaghan Urology Clinic, and their urine specimens were examined by two cytology methods (direct smear and LBC); also, their sensitivity and specificity were compared. The appropriate sample size was estimated from previous studies (20, 23).
All urine samples were collected at midday to prevent false-positive results (morning samples were not taken). The patients were advised to drink a few glasses of water 1-2 h before sampling. All samples were freshly voided urine. Urine samples were taken in our laboratory or immediately transferred to our laboratory; instrumented urine specimens were excluded. The gross nature of samples (such as color, volume, and clarity) was recorded. In our laboratory, each specimen was divided into two halves for further processing. One-half of the voided sample was prepared for the direct smear method and another half for the LBC method. To prevent cell damage, 10% formalin or 50% alcohol was equally added to the sample size immediately.
In the direct smear method, slide preparation was done by sediment obtained from centrifugation of urinary samples (1000 rpm for 30 min). The slide was stained with Papanicolaou and hematoxylin and eosin (H&E) staining methods.
In LBC, samples were centrifuged at 1500 rpm, and the precipitates were transferred to 30 mL of a Cytolytic solution (Sina Dej Sahand Co, Tabriz, Iran). After another round of centrifugation, two or three drops of precipitates were transferred to the preservative solution (Sina Dej Sahand Co, Tabriz, Iran). The vial and slide were placed in a ThinPrep processor (SHANDON, CYTOSPIN3, UK). The preparation steps are as follows: 1) dispersion: filter rotates within the sample vial, creating currents in the fluid that are strong enough to separate debris and disperse mucus but gentle enough to have no adverse effect on cell appearance; 2) cell collection: a gentle vacuum is created within the ThinPrep Filter, which collects cells on the exterior surface of the membrane; 3) cell transfer: after collecting the cells on the membrane, the ThinPrep Filter is inverted and gently pressed against the ThinPrep Microscope Slide. Natural attraction and slight positive air pressure cause the cells to adhere to the ThinPrep Microscope Slide, resulting in an even distribution of cells in a defined circular area. Then, ethanol 95% is used for fixation; and 4) staining: Papanicolaou and H&E staining methods were performed manually.
In both methods, the findings were reported according to the Paris System. Thereafter, all patients underwent cystoscopy and biopsy, and the precision of both cytology methods was compared according to biopsy results.
This study included all patients with suspicious symptoms and signs of bladder carcinoma or recurrent disease and all those patients with a history of bladder carcinoma referred for follow-up studies. We excluded patients with incomplete cytology, cystoscopy, and biopsy procedures from the study. Data collected from clinical and laboratory observations were analyzed using SPSS 21 (SPSS Inc., Chicago, Ill., USA). The clinical and laboratory characteristics of patients were described by descriptive statistical methods, and Student t-test, chi-square, McNemar, and Kappa tests were used. The sensitivity, specificity, positive, and negative predictive values of direct cytology and liquid-based methods were also calculated and compared based on final biopsy results.
All patients went through routine diagnostic and therapeutic procedures, and no additional diagnostic procedures were performed.
Here are some cytologic criteria that were used in our study to report:
Low-grade urothelial neoplasia (LGUN): three-dimensional cellular papillary clusters (defined as clusters of cells with nuclear overlapping, forming papillae) with fibrovascular cores, including capillaries.
Suspicious for high-grade urothelial carcinoma (SHGUC): this diagnosis is restrictively used in cases with abnormal urothelial cells that quantitatively fall short of a definitive diagnosis of high-grade urothelial carcinoma (HGUC).
HGUC: a cellular cytologic urine specimen with a minimum of five to ten viable malignant cells will qualify as HGUC (Figures 1 and 2).
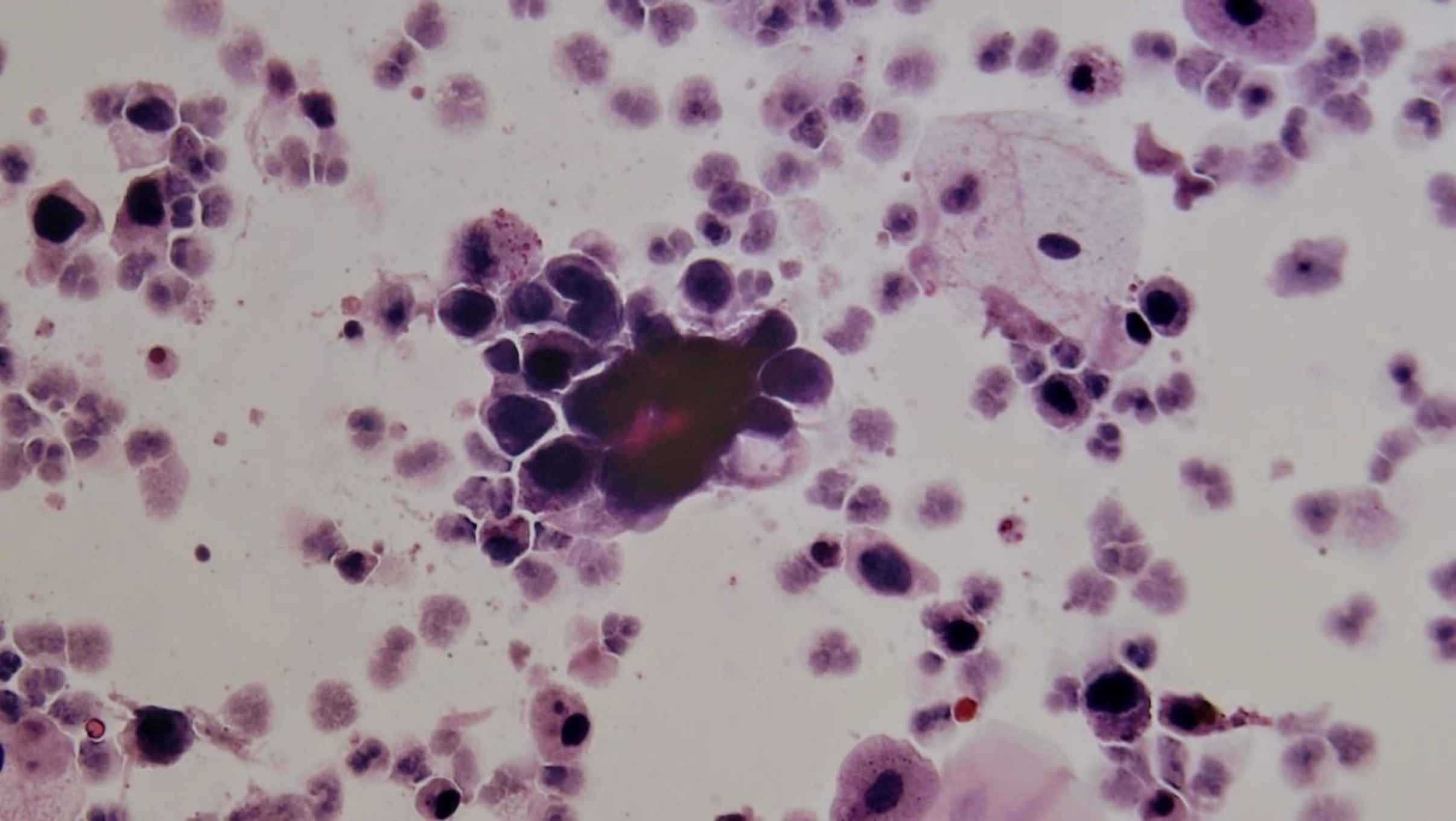
Fig. 1.Liquid-based cytology. HGUC: High-grade urothelial carcinoma
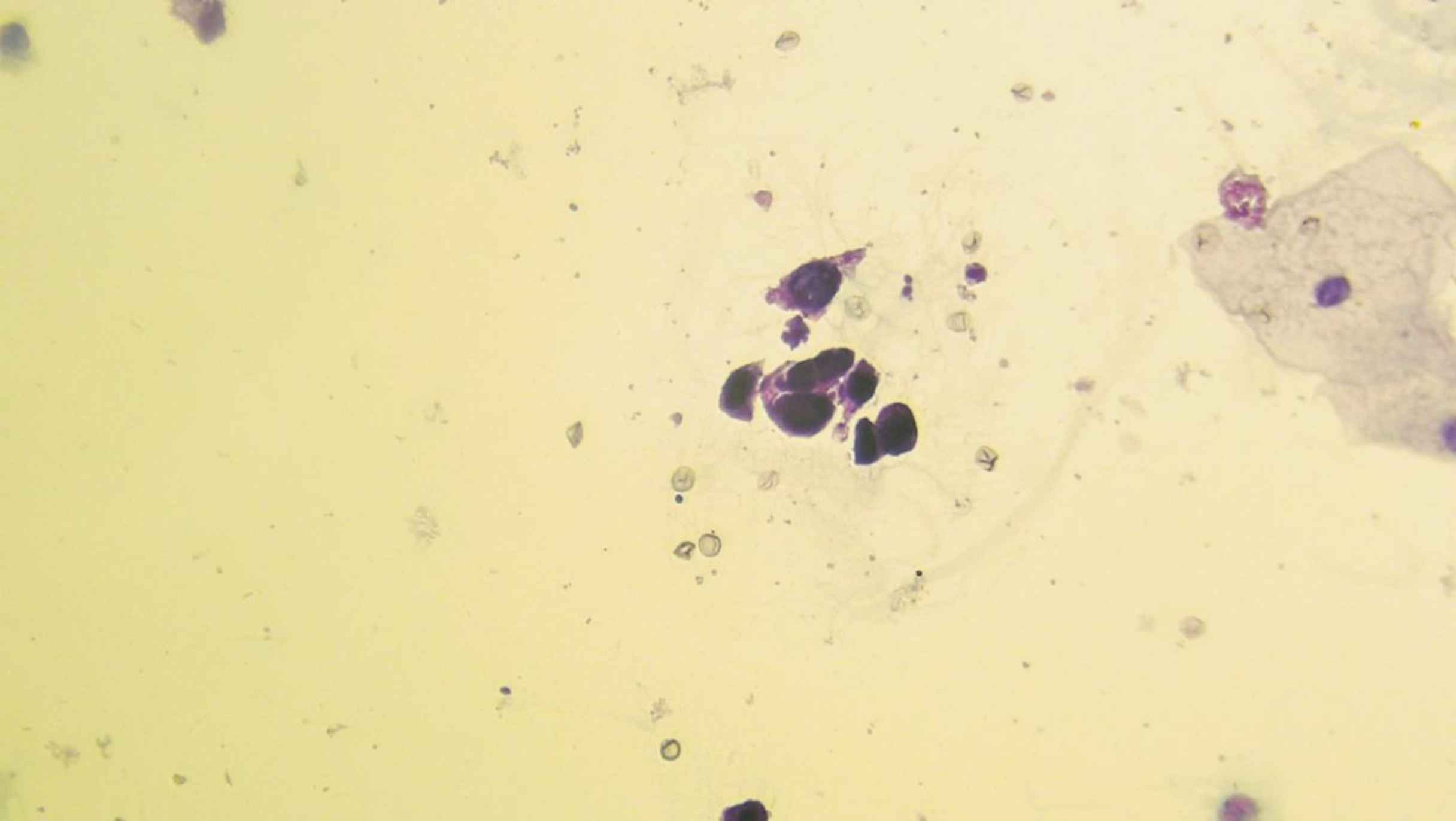
Fig. 2.Liquid-based cytology. HGUC: High-grade urothelial carcinoma
Atypical Urothelial cells (AUC): cellular changes that fulfill the major criterion (nuclear-cytoplasmic ratio >0.5) and only one minor criterion (nuclear hyperchromasia, irregular nuclear membranes, irregular, coarse, and clumped chromatin) (Figures 3 and 4).
No urothelial atypia or malignancy (NUAM): if any of the following components are present:
-Benign urothelial, glandular, and squamous cell
-Benign urothelial tissue fragments, sheets, or clusters
-Changes associated with lithiasis
-Viral cytopathic effect
-Post-therapy effect
Dysplasia: the urothelium shows markedly abnormal, enlarged, and hyperchromatic nuclei, though the degree of abnormality is somewhat less than in classic carcinoma in situ.
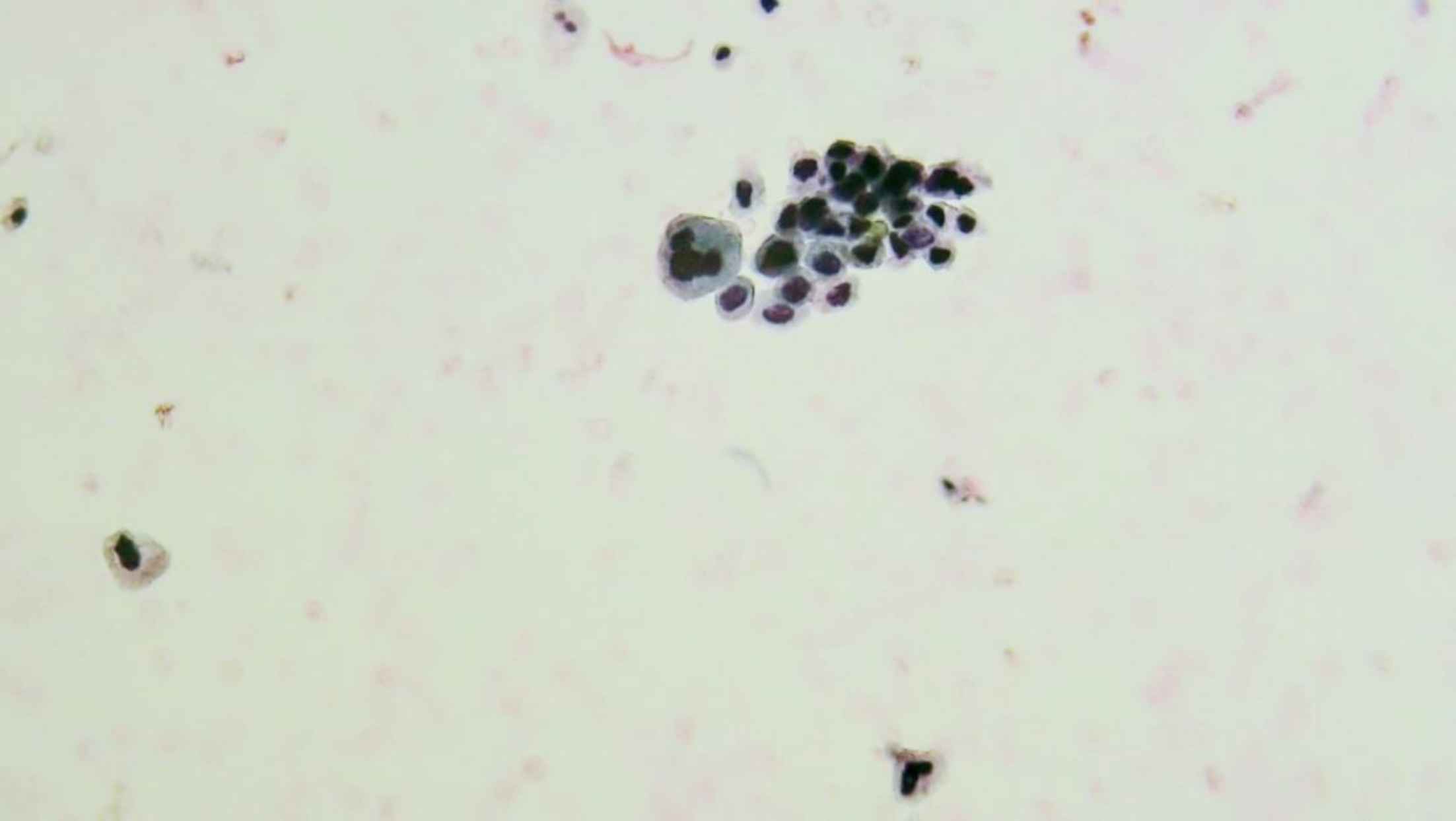
Fig. 3.Liquid-based cytology. AUC: Atypical urothelial cells
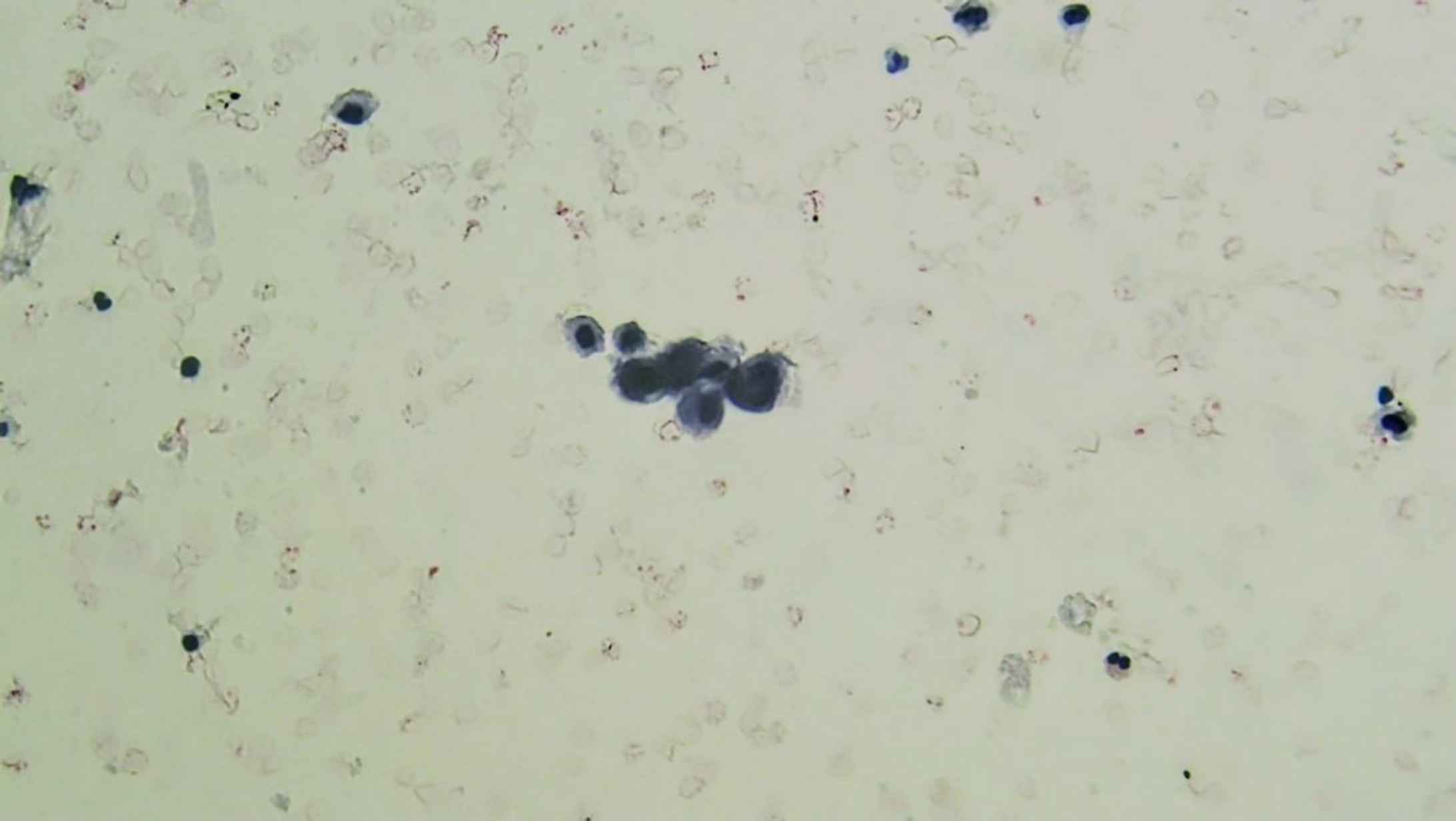
Fig. 4.Liquid-based cytology. AUC: Atypical urothelial cells
Results
A total of 146 patients were included in the study. Patients’ mean age was 61 years; 102 of them were male, and 44 were female.
The findings of the LBC and DSC methods are presented in Table 1. Biopsy findings are presented in Table 2.
The findings of DSC methods were compared with biopsy results (Table 3). The comparison results of biopsy and liquid-based cytology are depicted in Table 4. The accuracy of cytology methods was evaluated according to biopsy reports. The sensitivity and specificity of these two methods were also calculated (Table 5).
We compared biopsy results with LBC and DSC results; findings are as follows:
- High-grade Transitional Cell Carcinoma (HGT-CC) in biopsy: 13 out of 146 cases were HGTCC, 10 of which were invasive transitional cell carcinoma (INTCC). Of these 13 HGTCC biopsy cases, five were reported as HGUC in LBC (two HGUC and three SHGUC cases in DSC); four were reported as SHGUC in LBC (two HGUC and two SHGUC cases in DSC, which had severe hematuria); two were reported as AUC Figures 1 and 2 in LBC (one NUAM and one AUC cases in DSC, which were accompanied by severe inflammation). Two were reported as NUAM both in LBC and DSC methods.
- Low-grade transitional cell carcinoma (LGTCC) in biopsy: 10 of the biopsy results were LGTCC. Of these 10 LGTCC biopsy results, five were AUC in LBC (three AUC and two NUAM cases, all accompanied by hemorrhage); three were LGUN in LBC, all of which were AUC in DSC; and two were NUAM in LBC and in DSC, one of which had severe hematuria.
- Carcinoma in situ in biopsy: two cases of carcinoma in situ, both reported as HGUC in LBC and DSC.
- Dysplasia in biopsy: three cases of dysplasia were reported in biopsies, which were AUC in LBC and NUAM in DSC.
Moreover, the comparison of LBC results with DSC and biopsy results is presented in Table 6.
In this study, the largest difference was reported in patients with a diagnosis of AUC in the LBC method. In these 11 cases, six cases were reported as negative in DSC, one case was unsatisfactory, and only four cases were reported as AUC in the DSC method.
The biopsies of these 11 patients revealed 10 positive and only one negative report (with reactive changes due to radiotherapy). Therefore, in the McNemar test, there was a significant difference between the LBC and DSC methods in AUC patients (P=0.016).
Kappa statistics revealed a significant agreement between LBC and DSC in negative biopsy cases (P<0.000), Kappa value=0.663. However, there was poor agreement between the two methods in positive biopsies (P>0.05).
| Finding | LBC | DSC |
|---|---|---|
| NUAM | 121 (82.9%) | 119 (81.5%) |
| AUC | 11 (7.5%) | 6 (4.1%) |
| LGUN | 3 (2.1%) | 2 (1.4%) |
| SHGUC | 4 (2.7%) | 5 (3.4%) |
| HGUC | 7 (4.8%) | 6 (4.1%) |
| Total | 100% | 100% |
| Findings | Frequency | Percent |
|---|---|---|
| Negative | 118 | 80.8% |
| Dysplasia | 3 | 2.1% |
| CIS | 2 | 1.4% |
| LGTCC | 10 | 6.8% |
| HGTCC | 13 | 8.9% |
| Total | 146 | 100 |
| DSC finding | Frequency | Biopsy result:Negative (-) Positive (+) | |
|---|---|---|---|
| NUAM | 119 | 109 (91.6%) | 10 (8.4%) |
| AUC | 6 | 2 (33%) | 4 (66%) |
| LGUN | 2 | 2 (100%) | 0 |
| SHGUC | 5 | 0 | 5 (100%) |
| HGUC | 6 | 0 | 6 (100%) |
| Unsatisfactory | 8 | 7 (87.5%) | 1 (12.5%) |
| Total | 146 | 118 (80.8%) | 28 (19.2%) |
| LBC finding | Frequency | Biopsy result:Negative (-) Positive (+) | |
|---|---|---|---|
| NUAM | 121 | 117 (96.7%) | 4 (3.3%) |
| AUC | 11 | 1 (9.1%) | 10 (90.9%) |
| LGUN | 3 | 0 | 3 (100%) |
| SHGUC | 4 | 0 | 4 (100%) |
| HGUC | 7 | 0 | 7 (100%) |
| Total | 146 | 118 (80.8%) | 28 (19.2%) |
| DSC | LBC | |
|---|---|---|
| Sensitivity | 60.7% | 85.7% |
| Specificity | 98% | 99% |
| Positive Predictive Value | 89.4% | 96% |
| Negative Predictive Value | 91.3% | 96% |
| LBC | DSC | Biopsy |
|---|---|---|
| NUAM (N=6) | Dysplasia (N=3) LGTCC (N=2) HGTCC (N=1) | |
| AUC (N=11) | AUC (N=4) | LGTCC (N=2) HGTCC (N=1) Negative (N=1 , with reactive changes due to radiotherapy) |
| Unsatisfactory (N=1) | LGTCC (N=1) | |
| HGUC (N=7) | HGUC (N=4) | HGTCC (N=2) CIS (N=2) |
| SHGUC (N=3) | HGTCC (N=3) | |
| LGUN (N=3) | LGUN (N=2)AUC (N=1) | LGTCC (N=3) |
| SHGUC (N=4) | HGUC (N=2)SHGUC (N=2) | HGTCC (N=2) LGTCC (N=2) |
Discussion
Since 1939, screening of malignant neoplasms has relied on cytology. However, direct smear disadvantages (such as thick smear, overlapping cellular regions, low cellularity, inflammatory cells, red blood cells, and air bubble artifact) make the diagnosis difficult and result in low diagnostic sensitivity. Therefore, LBC has been introduced as a substitute for the conventional method and has been widely used over the past two decades (24-27). Several studies have compared DSC and LBC in fields other than gynecology. However, only a few studies have compared these two cytology techniques in urine specimens. In the analysis of 236 urine specimens conducted by Lee et al., it was shown that the use of a ThinPrep-based liquid-based preparation method was useful to improve the quality of the slides and reduce the duration of the test, but the sensitivity, accuracy, and predictive value were not changed (27).
In another study, Koh et al. pointed out that the use of CellPrepPlus LBC for body liquids had a higher sensitivity and higher negative predictive value. The quality of the slides was better than DSC (28). Therefore, it is a useful diagnostic method in body fluid screening.
Conventional urine cytology methods include cell centrifugation (cytospin), Millipore filtration, and DSC. In the cytospin method, it may be associated with low cellularity and non-uniform cells throughout the slide or highly cellular smears with poor cell preparation. Contrary to urine cytology, in other fields (gynecology and non-gynecology), the conventional method of slide preparation generally has no problem with low cellularity. In contrast, highly cellular content requires more screening time due to the increased number of slides in each sample and analysis of different cell regions (28, 29).
In the LBC method, the cells are washed with a liquid and processed automatically. Compared to DSC, LBC shows less vague elements, while the cytological characteristics of cells are preserved. Therefore, LBC solves one of the major problems in urine cytology, which is the low cellularity (14).
In our study, a total of 146 samples were taken from patients suspected of bladder carcinoma and examined by both DSC and LBC. The sensitivity and specificity in DSC were 60.7% and 98% and in LBC were 85.7% and 99%, respectively. However, in Fakhrjoo et al.’s study, the sensitivity and specificity of DSC in the diagnosis of bladder tumors of 900 patients were 73% and 99%, respectively (20).
In 2009, Lu et al. compared CellPrepPlus LBC with the conventional smear in 713 patients. The diagnostic sensitivity for CellPrepPlus was 50% and higher than 37.5% for the conventional smear. The specificity of both preparations was 100% (17).
In our study, the positive predictive value was 89.4%, and the negative predictive value was 91.3% for DSC and 96% for LBC. We thought that the difference between other studies (20, 24) and ours is due to different processing methods, which preserve cytological characteristics of cells. We used ThinPrep for processing our specimens but, in most of the other studies, CellPrep was used. Other causes are various LBC diagnostic definitions, different sample sizes, and pathologists’ skills.
In our study, the biggest difference was in the AUC group (11 cases in LBC and six cases in DSC). In the LBC group, 10 out of 11 had positive biopsy results, and there was only one negative biopsy due to radiotherapy.
The McNemar test showed a significant difference between LBC and DSC (P=0.016). This difference was because of eliminating cellular debris, inflammatory cells, and red blood cells, as well as the preservation of cytological characteristics in the LBC method, which made the diagnosis easier. On the other hand, in AUC, the pathologist detected mild malignant cytologic changes; therefore, the omission of background elements was very helpful. However, in higher malignant grades, changes can be detectable in DSC, even in the presence of disturbing background elements.
Kappa statistics revealed a significant agreement between LBC and DSC in negative biopsy cases (P<0.000), Kappa value=0.663.
However, there was poor agreement between the two methods in positive biopsies (P>0.05). This finding shows that LBC is preferable to DSC in detecting positive cases and malignant cells due to lower background elements. LBC reduces unsatis-factory cases, which is not uncommon in the DSC method. In France, Piaton et al. (2005) examined 79 urine samples and found no significant difference between the LBC (ThinPrep) and DSC methods in the diagnosis of nuclear abnormalities (P=0.01) (30). In our study regarding nuclear abnormalities, there was no significant difference between the DSC and LBC methods, but the LBC method helped us to improve cell-free background; therefore, we managed to have lower AUC cases.
Kapoor et al. concluded that LBC offered better detection of malignant cells in the urine of patients with bladder tumors than DSC. Moreover, the detection of malignant cells by LBC was even better in the background of hematuria (31). These findings are similar to our results
Conclusion
This study shows higher sensitivity and higher specificity of Thinprep liquid-based cytology than direct smear cytology, especially in the diagnosis of Urothelial tumors with low-grade malignancy. LBC method can reduce AUC cases which is the waste-basket for pathologists. Furthermore, it lowers the unsatisfactory cases in DSC. In conclusion, although the LBC method costs more, its several advantages over the DSC method make it an appropriate alternate method to evaluate urinary samples.
Conflict of Interest
The authors declared no conflict of interest.
Funding
This study was supported by Mashhad University of Medical Sciences, Mashhad, Iran.
Acknowledgments
Special thanks to the staff of Armaghan urology clinic and Ghaem hospital (pathology department) for their excellent technical assistance.
References
- Eble JN SG, Epstein JI, Sesterhenn I. World Health Organization classification of tumors. Pathology and genetics of tumours of the urinary system and male genital organs. lyon: IARC Press; 2005.
- Inamura K. Bladder Cancer: New Insights into Its Molecular Pathology. Cancers (Basel).. 2018; 10:4.
- Pasin E, Josephson DY, Mitra AP, Cote RJ, Stein JP. Superficial bladder cancer: an update on etiology, molecular development, classification, and natural history. Rev Urol.. 2008; 10(1):31-43.
- Zieger K, Wolf H, Olsen PR, Hojgaard K. Long-term follow-up of noninvasive bladder tumours (stage Ta): recurrence and progression. BJU Int.. 2000; 85(7):824-8.
- Heney NM, Ahmed S, Flanagan MJ, Frable W, Corder MP, Hafermann MD. Superficial bladder cancer: progression and recurrence. J Urol.. 1983; 130(6):1083-6.
- Kiemeney LA, Witjes JA, Verbeek AL, Heijbroek RP, Debruyne FM. The clinical epidemiology of superficial bladder cancer. Dutch South-East Cooperative Urological Group. Br J Cancer.. 1993; 67(4):806-12.
- Han RF, Pan JG. Can intravesical bacillus Calmette-Guérin reduce recurrence in patients with superficial bladder cancer? A meta-analysis of randomized trials. Urology.. 2006; 67(6):1216-23.
- Anastasiadis A, de Reijke TM. Best practice in the treatment of nonmuscle invasive bladder cancer. Ther Adv Urol.. 2012; 4(1):13-32.
- Zhu CZ, Ting HN, Ng KH, Ong TA. A review on the accuracy of bladder cancer detection methods. J Cancer.. 2019; 10(17):4038-44.
- Wiener HG, Mian C, Haitel A, Pycha A, Schatzl G, Marberger M. Can urine bound diagnostic tests replace cystoscopy in the management of bladder cancer? J Urol.. 1998; 159(6):1876-80.
- Stamatiou K, Papadoliopoulos I, Dahanis S, Zafiropoulos G, Polizois K. The accuracy of ultrasonography in the diagnosis of superficial bladder tumors in patients presenting with hematuria. Ann Saudi Med.. 2009; 29(2):134-7.
- Ozen H, Hall MC. Bladder cancer. Curr Opin Oncol.. 2000; 12(3):255-9.
- Truta A, Popon TA, Saraci G, Ghervan L, Pop IV. Novel non invasive diagnostic strategies in bladder cancer. Clujul Med.. 2016; 89(2):187-92.
- Hoda RS. Non-gynecologic cytology on liquid-based preparations: A morphologic review of facts and artifacts. Diagn Cytopathol.. 2007; 35(10):621-34.
- Planz B, Jochims E, Deix T, Caspers HP, Jakse G, Boecking A. The role of urinary cytology for detection of bladder cancer. Eur J Surg Oncol.. 2005; 31(3):304-8.
- Linder J. Recent advances in thin-layer cytology. Diagn Cytopathol.. 1998; 18(1):24-32.
- Lu DY, Nassar A, Siddiqui MT. High-grade urothelial carcinoma: comparison of SurePath liquid-based processing with cytospin processing. Diagn Cytopathol.. 2009; 37(1):16-20.
- V L. Diagnostic Cytopathology. Churchill Livingstone; 2010.
- Denton KJ. Liquid based cytology in cervical cancer screening. Bmj.. 2007; 335(7609):1-2.
- Fakhrjou a, madaen sk. Specificity and sensitivity of urine cytology for screening patients with urothelial tumors and hematuria. Medical journal of tabriz university of medical sciences.. 2003; 37(57)
- Kord S, Mokhtari M, Tahmasebi S. Comparison of Liquid-based and Conventional Cytology in Diagnosis of Breast Mass. J Cytol.. 2019; 36(1):22-7.
- Deshou H, Changhua W, Qinyan L, Wei L, Wen F. Clinical utility of Liqui-PREP™ cytology system for primary cervical cancer screening in a large urban hospital setting in China. J Cytol.. 2009; 26(1):20-5.
- Son SM, Koo JH, Choi SY, Lee HC, Lee YM, Song HG. Evaluation of Urine Cytology in Urothelial Carcinoma Patients: A Comparison of CellprepPlus® Liquid-Based Cytology and Conventional Smear. Korean J Pathol.. 2012; 46(1):68-74.
- Koo JH, Lee HC, Song HG, Han HS, Lee KH, Choe KH. Comparison of Cytologic Evaluation between Conventional Method and CellprepPlus(R) Liquid-Based Cytology in Body Fluid. J Pathol Transl Med.. 2009; 43(5):448-52.
- Gibb RK, Martens MG. The impact of liquid-based cytology in decreasing the incidence of cervical cancer. Rev Obstet Gynecol.. 2011; 4(Suppl 1):S2-s11.
- Karnon J, Peters J, Platt J, Chilcott J, McGoogan E, Brewer N. Liquid-based cytology in cervical screening: an updated rapid and systematic review and economic analysis. Health Technol Assess.. 2004; 8(20):iii, 1-78.
- Lee S, Park JH, Do SI, Kim YW, Lee J, Chang SG. Diagnostic Value of Urine Cytology in 236 cases; a Comparison of Liquid-Based Preparation and Conventional Cytospin Method. J Pathol Transl Med.. 2007; 18(2):119-25.
- Koh JS, Cho SY, Ha HJ, Kim JS, Shin MS. Cytologic Evaluation of CellPrep(R) Liquid-based Cytology in Cervicovaginal, Body Fluid, and Urine Specimens: Comparison with ThinPrep(R). J Pathol Transl Med.. 2007; 18(1):29-35.
- Yim H, Joo HJ, Kim YB, Hong SW. Comparison of Conventional Smear, Cell Block and Liquid-based Preparation in the Evaluation of Bronchial Washing Specimen in Lung Cancer Patients. J Pathol Transl Med.. 2011; 45(3):296-302.
- Piaton E, Faÿnel J, Hutin K, Ranchin MC, Cottier M. Conventional liquid-based techniques versus Cytyc Thinprep processing of urinary samples: a qualitative approach. BMC Clin Pathol.. 2005; 5:9 .
- Kapoor K, Datta C, Pal DK. Is liquid-based cytology an alternative to conventional cytology for detection of malignant cells in urine of bladder cancer? Eastern Indian prospective observational study. Turk J Urol.. 2019; 45(5):351-6.

